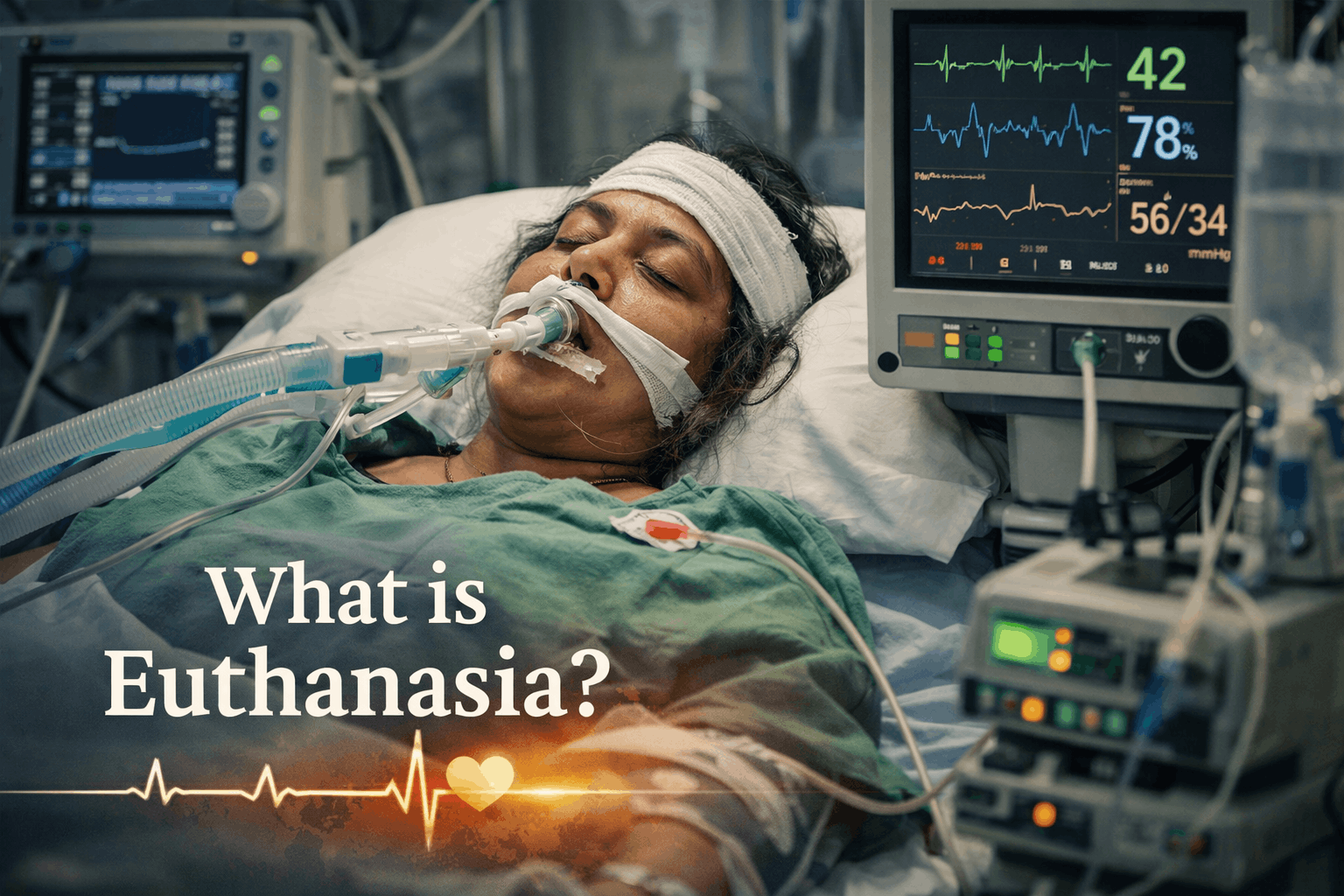
1. Introduction
What is Euthanisa? is most essential question to understand life, law and dignity of a person. Advances in modern medicine have dramatically increased human life expectancy. However, these same medical technologies have also created complex ethical dilemmas regarding the prolongation of life in circumstances where recovery is medically impossible. Patients suffering from terminal illnesses, irreversible comas, or persistent vegetative states often face prolonged suffering sustained by life-support systems. In such situations, the question arises whether individuals should have the right to refuse life-sustaining treatment or seek assistance in ending unbearable suffering.
This dilemma lies at the heart of the debate surrounding euthanasia. Across the world, legal systems, medical professionals, philosophers, and religious communitises continue to grapple with the question of whether ending life under certain circumstances can ever be morally or legally justified. The issue is not merely about death; it concerns broader principles such as bodily autonomy, human dignity, medical ethics, and the role of the state in regulating life-and-death decisions.
In India, the debate gained national attention following cases involving patients in irreversible medical conditions, where families and doctors faced difficult choices about continuing life-support treatment. Judicial recognition of the concept of “dying with dignity” under the constitutional right to life has further intensified discussions on end-of-life decision-making.
Euthanasia therefore represents one of the most complex intersections of law, medicine, ethics, and human dignity. Understanding its meaning, types, ethical arguments, and legal status across jurisdictions is essential for evaluating ongoing debates in India and globally.
2. What is Euthanasia? Defination & Meaning
The term euthanasia originates from the Greek words eu meaning “good” and thanatos meaning “death.” Literally translated, euthanasia means “good death” or “easy death.” Historically, the concept referred to dying peacefully without unnecessary suffering.
In contemporary medical and legal discourse, euthanasia generally refers to the intentional termination of a person’s life to relieve suffering caused by serious and incurable illness.
Scholars define euthanasia in slightly different ways depending on ethical and legal contexts. According to bioethicist Tom L. Beauchamp, euthanasia involves an act or omission carried out with the intention of ending a patient’s life for the patient’s benefit. Similarly, legal literature often describes euthanasia as the deliberate intervention undertaken by medical professionals or others to end life in order to relieve unbearable suffering.
From a legal perspective, euthanasia raises questions about consent, intention, and the role of medical practitioners. Many legal systems distinguish euthanasia from suicide and from withdrawal of medical treatment, even though these issues often overlap in practical situations.
It is therefore necessary to examine the different forms euthanasia can take.
3. Historical Development of the Concept
Debates about euthanasia are not new. Discussions regarding the morality of ending life in situations of suffering can be traced to ancient philosophical traditions.
In ancient Greek thought, philosophers such as Plato and Socrates discussed the idea that individuals suffering from incurable illness might reasonably choose death. However, Hippocratic medical ethics generally opposed physicians intentionally causing death. The famous Hippocratic Oath explicitly stated that physicians should not administer deadly drugs even if requested by patients.
During the medieval period, religious doctrines strongly influenced medical ethics. Christian theology emphasised the sanctity of life and regarded the deliberate termination of life as morally unacceptable. As a result, euthanasia was largely condemned throughout medieval European societies.
The modern debate re-emerged in the nineteenth and twentieth centuries as medical science advanced. Life-support technologies such as ventilators and artificial nutrition made it possible to sustain biological life even when consciousness or recovery was impossible. These developments raised new questions about whether prolonging life at all costs was ethically justified.
In the late twentieth century, bioethics emerged as a specialised field addressing ethical issues in medicine and biotechnology. Scholars began to analyse euthanasia using frameworks based on autonomy, dignity, and patient rights. Court cases in various countries further shaped the legal discourse on euthanasia and assisted dying.
Today, euthanasia remains a subject of intense ethical and legal debate worldwide.
4. Types of Euthanasia
Euthanasia is not a single practice but a group of related actions that differ in intention, consent, and medical procedure. Legal systems often distinguish between several types.
i. Active Euthanasia
Active euthanasia occurs when a person deliberately performs an action that directly causes the death of a patient. This may involve administering a lethal injection or medication with the intention of ending life.
Active euthanasia is controversial because the medical practitioner directly causes death. Most countries prohibit active euthanasia, although some jurisdictions such as the Netherlands and Belgium permit it under strict legal conditions.
ii. Passive Euthanasia
Passive euthanasia involves withholding or withdrawing life-sustaining medical treatment, allowing the patient to die naturally from their underlying illness. Examples include discontinuing ventilator support or stopping artificial nutrition.
Many legal systems view passive euthanasia differently from active euthanasia because the doctor does not directly cause death but allows the disease to take its natural course. Courts in several countries have recognised a patient’s right to refuse medical treatment, including life-support measures.
iii. Physician-Assisted Dying
Physician-assisted dying occurs when a doctor provides a patient with the means to end their own life, usually by prescribing lethal medication. The final act is performed by the patient rather than the physician.
This model is legally permitted in several jurisdictions, including certain states in the United States and Canada. The practice is typically regulated through strict safeguards such as psychiatric evaluations and multiple consent requirements.
iv. Voluntary, Non-Voluntary, and Involuntary Euthanasia
Another classification focuses on the presence or absence of patient consent.
Voluntary euthanasia occurs when a competent patient explicitly requests assistance in dying.
Non-voluntary euthanasia occurs when the patient is incapable of expressing consent, such as in cases of coma or severe brain injury. Decisions are made by family members or medical authorities.
Involuntary euthanasia occurs when life is ended against the patient’s wishes. This is widely condemned as unethical and illegal.
These distinctions are crucial because most legal frameworks only consider voluntary euthanasia or physician-assisted dying under strict conditions.
5. Medical Context: When Does the Debate Arise?
Euthanasia debates generally arise in situations where patients face severe and irreversible medical conditions. Several medical scenarios frequently appear in legal and ethical discussions.
Terminal Illness
Patients suffering from advanced cancer, neurodegenerative diseases, or other terminal illnesses may experience intense pain and loss of bodily function. In such circumstances, some patients request assistance in dying to avoid prolonged suffering.
Persistent Vegetative State (PVS)
A persistent vegetative state refers to a medical condition where a patient loses cognitive function but retains basic physiological functions such as breathing and circulation. Patients in PVS may remain alive for years through artificial feeding and medical support.
Irreversible Coma
Patients in irreversible coma have no awareness or responsiveness and cannot regain consciousness. Decisions regarding continuation or withdrawal of life support become particularly complex in such cases.
Life-Sustaining Technology
Modern medicine has developed numerous technologies capable of prolonging life, including ventilators, dialysis machines, and artificial nutrition. While these technologies can save lives, they also raise ethical questions when they merely prolong suffering without the possibility of recovery.
Thus, euthanasia debates often revolve around the appropriate limits of medical intervention.
6. Ethical Debate
The ethical debate surrounding euthanasia is multifaceted and deeply polarised.
i. Autonomy and Self-Determination
Supporters of euthanasia argue that individuals have a fundamental right to control their own bodies and medical decisions. Respecting patient autonomy means allowing competent adults to decide when medical treatment should end.
This argument emphasises the principle of personal liberty and self-determination in healthcare.
ii. Sanctity of Life
Opponents argue that human life possesses intrinsic value and should not be intentionally destroyed. Religious traditions often emphasise that life is sacred and that deliberately ending it undermines moral and social foundations.
From this perspective, legalising euthanasia risks weakening societal respect for human life.
iii. Compassion and Relief from Suffering
Another ethical argument emphasises compassion. Supporters claim that when patients experience unbearable suffering with no hope of recovery, assisting death may represent an act of mercy rather than cruelty.
Palliative care advocates, however, argue that improved pain management and end-of-life care can alleviate suffering without ending life.
iv. Risk of Misuse and Vulnerable Populations
Critics also warn that legalising euthanasia could endanger vulnerable individuals such as the elderly, disabled, or economically disadvantaged. Concerns exist that subtle social pressure might influence patients to choose death to avoid being a burden on their families.
These ethical concerns have significantly influenced legal approaches worldwide.
7. Global Legal Approaches
Different countries have adopted varied legal responses to euthanasia.
Netherlands
The Netherlands became the first country to legalise euthanasia in 2002. Physicians may perform euthanasia if strict conditions are satisfied, including voluntary request, unbearable suffering, and consultation with another physician.
Belgium
Belgium also legalised euthanasia in 2002. The law allows euthanasia for adults suffering from serious and incurable illness under specific safeguards.
Canada
Canada legalised physician-assisted dying through the Medical Assistance in Dying (MAiD) legislation in 2016. The law permits doctors to assist patients with grievous and irremediable medical conditions.
United States
In the United States, euthanasia remains illegal at the federal level, but physician-assisted dying is permitted in several states such as Oregon, Washington, and California under “Death with Dignity” laws.
United Kingdom
The United Kingdom maintains a strict prohibition on euthanasia and assisted suicide under the Suicide Act 1961. However, courts have acknowledged the right of competent patients to refuse medical treatment.
These varying approaches demonstrate the complexity of balancing autonomy, ethics, and public policy.
8. Emerging Debate in India
In India, the debate on euthanasia has largely evolved through judicial decisions rather than legislative reforms. The Supreme Court has interpreted the constitutional right to life under Article 21 to include elements of dignity and personal autonomy.
A landmark turning point occurred in the Aruna Shanbaug case, where the Supreme Court allowed passive euthanasia under specific judicial supervision. Later, the Court recognised the validity of living wills and advance directives, allowing individuals to express their wishes regarding end-of-life medical treatment.
These decisions marked a significant shift in Indian constitutional jurisprudence, acknowledging that the right to life also includes the right to die with dignity in certain circumstances.
However, India still prohibits active euthanasia, and the legal framework continues to evolve through judicial interpretation and policy discussions.
9. Conclusion
Euthanasia represents one of the most challenging moral and legal questions confronting modern societies. Advances in medical technology have made it possible to prolong life in circumstances where recovery may be impossible, forcing societies to reconsider the boundaries between life preservation and human dignity.
The debate involves competing ethical principles including autonomy, sanctity of life, compassion, and protection of vulnerable populations. Different legal systems have adopted varied approaches, ranging from strict prohibition to carefully regulated forms of assisted dying.
In India, judicial recognition of passive euthanasia and living wills reflects an evolving understanding of dignity within the constitutional right to life. Nevertheless, many ethical, medical, and legal questions remain unresolved.
As medical technologies continue to advance, societies will need to develop nuanced frameworks that respect both human dignity and the value of life. Understanding euthanasia in its historical, ethical, and legal contexts is therefore essential for informed public debate and future legal reforms.
This discussion also sets the stage for examining how Indian law has developed specific doctrines governing end-of-life decisions.
Quick Summary
- Euthanasia refers to intentionally ending life to relieve suffering caused by severe and incurable illness.
- The concept includes different forms such as active euthanasia, passive euthanasia, and physician-assisted dying.
- Ethical debates focus on autonomy, sanctity of life, compassion, and risks of misuse.
- Legal approaches vary worldwide, with some countries allowing regulated assisted dying while others prohibit it.
- In India, passive euthanasia and living wills have been recognised by the Supreme Court under the right to dignity within Article 21.
Life, Law and Dignity : Understanding Euthansia Series
The next article in this series would find as below:
- What is Euthanasia? Understanding the Concept, Types, and Global Legal Debate
- The Legal Journey of Euthanasia in India: From Aruna Shanbaug to the Right to Die with Dignity, The Legal Evolution of Euthanasia in India
- Vegetative State, Living Wills, and Medical Ethics: When Does Life-Sustaining Treatment Become Futile?
- The Harish Rana Case and Passive Euthanasia in India: A New Chapter in End-of-Life Law
- The Future of End-of-Life Law in India: Should Parliament Enact a Comprehensive Euthanasia Law?
References
- Tom L. Beauchamp & James F. Childress, Principles of Biomedical Ethics (7th ed. 2013).
- Helga Kuhse & Peter Singer, Bioethics: An Anthology (2d ed. 2006).
- Margaret Pabst Battin, Ending Life: Ethics and the Way We Die (2005).
- Jonathan Herring, Medical Law and Ethics (9th ed. 2021).
- Emily Jackson, Medical Law: Text, Cases, and Materials (5th ed. 2019).
- James Rachels, Active and Passive Euthanasia, 292 New Eng. J. Med. 78 (1975).
- John Keown, Euthanasia, Ethics and Public Policy, 11 Cambridge Q. Healthcare Ethics 345 (2002).
- Margaret Pabst Battin, Physician-Assisted Suicide and Euthanasia, 7 J. Med. Ethics 79 (1981).
- World Health Organization, Ethics and Health: End-of-Life Care (World Health Org. 2017).
- Government of Canada, Medical Assistance in Dying (MAiD) Legislation, Department of Justice (2016).
- Aruna Ramachandra Shanbaug v. Union of India, (2011) 4 S.C.C. 454 (India).
- Common Cause v. Union of India, (2018) 5 S.C.C. 1 (India).
- India Const. art. 21.
- Indian Kanoon, https://indiankanoon.org.